From federal budget threats to tech-powered care delivery, here’s what EMS directors and prehospital leaders need to know—and do next.
Emergency Medical Services is at a turning point.
EMS providers are facing a perfect storm of financial strain, policy shifts, and growing expectations, including the ask to solve problems that go far beyond transport.
But amid the noise, Pinnacle 2025 surfaced a clear message: EMS is more than just a ride. It’s a critical part of the healthcare continuum.
This year’s conference touched on several key themes, including reimbursement reform, hospital partnerships, smarter technology, and a louder political voice. Here’s what stood out—and why it matters now.
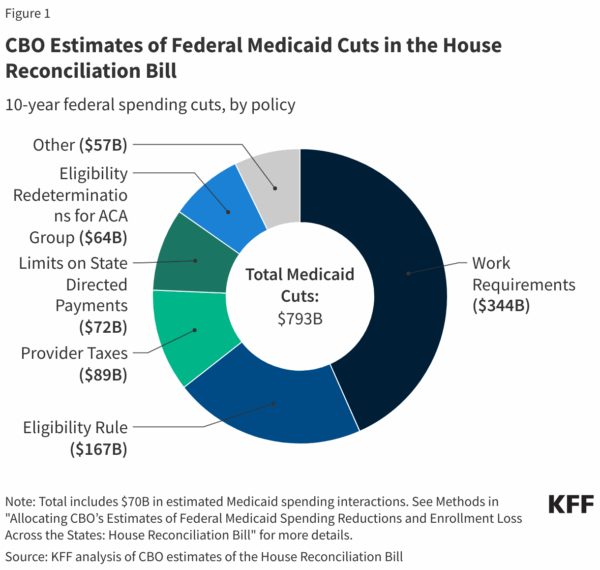
The Big, Beautiful Bill: What federal cuts could mean for EMS
The proposed federal budget (aka the “Big, Beautiful Bill”) threatens sweeping changes to Medicaid and ACA subsidies. According to the Kaiser Family Foundation, 12 million people could lose Medicaid coverage, with another 4 million impacted by the expiration of premium tax credits.
Why does this matter for EMS teams?
Because more uninsured patients means more uncompensated care. Hospitals, already under strain, could become less willing to fund partnerships unless EMS can prove real value. And with site-neutral payment reforms slashing outpatient reimbursements, the pressure will only grow.
The budget cuts are still three years out, but EMS leaders can’t afford to wait and see where the chips fall. The time to prepare is now. Build stronger relationships with hospitals. Track outcomes. Show how your work drives efficiency—not just transport.
A rare shot at rural transformation
For once, the funding window is open—and EMS has a chance to shape how it’s used.
The new $50B Rural Health Transformation Program provides $100M per state annually, with additional funds distributed at the discretion of CMS. But here’s the catch: states must submit their transformation plans by the end of 2025. That means EMS leaders across the country have a short—but real—opportunity to lobby for inclusion.
This funding isn’t just about rides. It could also support:
- Community paramedicine
- Mobile integrated health (MIH)
- Workforce training and retention
- Transport to alternative destinations
Positioned well, EMS can become the vital connector between rural communities and urban hospitals—driving down costs, boosting access, and securing sustainable reimbursement.
Hospital-at-Home: How EMS plays a key role in unblocking hospital capacity
Sean Kukauskas, Executive Director of Mass General Brigham Ambulance Services, shared how their Hospital-at-Home model has transformed not just where care happens, but how it directly affects throughput and length of stay.
In 2024, Mass General Brigham faced massive capacity constraints, which lead to the decline of over 1000 inpatient transfers from the community. Implementing the Hospital-at-Home program didn’t just expand capacity—it shortened inpatient stays by as much as 4 to 5 days.
EMS isn’t a side player in this model; it’s essential. Transport is Medicare Part A billable and bundled into the hospital stay, providing a steady reimbursement stream and removing billing friction. That’s why Mass General is actively encouraging EMS partnerships to support both emergent and scheduled home-based care. Kukauskas put it plainly: “Non-emergent and emergent transportation can be a single point of failure for patient throughput.”
“Non-emergent and emergent transportation can be a single point of failure for patient throughput.”
– Sean Kukauskas, Executive Director, Mass General Brigham Ambulance Services
For EMS agencies looking to diversify revenue and strengthen hospital ties, this is the time to start a conversation around how to support Mobile Integrated Healthcare (MIH) programs that expand care outside the four walls of the hospital.
Why the ET3 model stalled, and what EMS should do next
At Pinnacle’s session on the Emergency Triage, Treat, and Transport (ET3) Model, Brenda Staffan of Priority OnDemand and Reid Kiser of Kiser Healthcare Solutions unpacked why the program didn’t live up to its potential—and what that says about where EMS goes next.
The idea behind ET3 was bold: give EMS the tools to treat in place or take patients to alternative destinations instead of defaulting to the emergency department. But limited buy-in, payer resistance, the arrival of the COVID-19 pandemic, and a lack of measurable ROI meant the model never scaled.
Still, Staffan and Kiser emphasized that the failure wasn’t about the concept. It was about timing, trust, and infrastructure. ET3 showed what’s possible—and where EMS leaders can—and should—go next:
- Empower medics with protocols and payer-aligned incentives
- Build trust with ACOs and managed care plans
- Document the value of non-ED care pathways
As Medicare Advantage enrollment continues to outpace traditional Medicare, EMS agencies will need to speak the language of outcomes and value-based care in ways that make sense to payers.
Smarter data, stronger decisions
“Healthcare is the only industry that has added technology and seen negative productivity.”
That quote from Eric Beck, President & CEO of ESO, during the session “Unlocking the Black Box: Leveraging Data Science for Smarter Public Safety Decisions,” summed up a core challenge facing EMS leaders today. Alongside Todd Stout (Founder & President of FirstWatch) and Guillermo Fuentes (COO, Fitch & Associates), Beck outlined a persistent issue: when agencies invest in technology built primarily for end-user functionality, they often create a “black box” of back-end data, rich with insight but rarely used.
Instead, agencies need to treat their tech infrastructure not just as a set of operational tools, but as the foundation for data-driven outcomes. That starts with connecting disparate systems—CAD, dispatch, records, hospital outcomes—to uncover trends, inform protocols, and make smarter, more responsive decisions.
Todd Stout shared a powerful example of this kind of data integration and analysis. A recent pilot used fire department CAD data and school records to identify students who may have experienced traumatic events. This initiative creates opportunities for early intervention and mental health support before those students even arrive at school the next morning.
Meanwhile, ESO, in collaboration with Johns Hopkins, partnered with eight EMS agencies to build a data-driven framework for improving 911 response prioritization (one more accurate than traditional determinant levels.) Their research, published in this white paper, revealed that not all low-acuity calls are actually low risk. In fact, some ALPHA-level protocols included a surprising proportion of time-critical interventions.
These insights have real operational implications. With the right thresholds, up to 8% of EMS requests could be safely referred to alternative resources or deferred for non-emergent dispatch—without compromising safety.
Ultimately, the real challenge isn’t in adopting new technology, it’s about using it wisely. Integrated systems, analytics tools, and reporting structures must be designed to drive outcomes, not just compliance.
“Healthcare is the only industry that has added technology and seen negative productivity.”
– Eric Beck, President & CEO, ESO
EMS is more than “just a ride”
One panel of industry association leaders identified staffing and retention as two major issues keeping EMS leadership up at night. But perhaps more surprisingly, the third issue was perception. Too often, EMS is seen as a vehicle and not a clinical partner. As one panelist put it, “In 20 years, I want patients to thank us for the care we gave, not just the ride we provided.”
To get there, EMS teams must:
- Speak with one voice through national and state associations
- Push for reimbursement that reflects clinical value
- Continue innovating with MIH and preventive care—even when reimbursement is unclear
Funding and recognition both matter. EMS leadership shouldn’t only be part of the conversation when something goes wrong.
The 4 actions you should take now
Pinnacle EMS 2025 wasn’t just a download of industry news—it was a call to lead. If you’re in EMS or prehospital services leadership, here’s where to start:
- Get involved in your state’s Rural Transformation Plan. Advocate for EMS inclusion before the swiftly approaching December 2025 deadline.
- Partner with hospitals exploring Hospital-at-Home models. These programs need EMS partners—and they pay accordingly.
- Engage with policy associations. AAA, NAEMT, and other associations are pushing legislation that affects your bottom line.
- Track your impact. Whether it’s stroke triage or response time, data is the bridge between what you do and what others see, and the best way to prove your worth.
Redefining the future of EMS
The pressures on EMS aren’t easing up—budget threats, capacity crunches, tech growing pains. But there’s also real momentum.
Pinnacle 2025 did more than spotlight these challenges. It offered EMS leaders a way forward. Seize this moment – with clarity, creativity, and collaboration – and savvy leaders will be seem as more than “just ride.” Instead, you can be a partner in care, a leader in innovation, and a force for public health transformation.